Outlook for Stem Cell Therapy: its role in tendon regeneration
/By Dr Debbie Guest
Tendon injuries occur very commonly in racing thoroughbreds and account for 46% of all limb injuries. The superficial digital flexor tendon (SDFT) is the most at risk of injury due to the large strains that are placed upon it at the gallop. Studies have reported that the SDFT experiences strains of up to 11-16% in a galloping a thoroughbred, which is very close to the 12-21% strain that causes the SDFT to completely rupture in a laboratory setting.
An acute tendon injury leads to rupture of the collagen fibres and total disruption of the well organised tendon tissue (Figure 1). There are three phases to tendon healing: an inflammatory phase that lasts for around one week, where new blood vessels bring in large numbers of inflammatory blood cells to the damaged site—a proliferative phase that lasts for a few weeks, where the tendon cells rapidly multiply and start making new collagen to replace the damaged tissue; and a remodelling phase that can last for many months, where the new collagen fibres are arranged into the correct alignment and the newly made structural components are re-organised.
Figure 1. A) The healthy tendon consists predominantly of collagen fibres (light pink), which are uniformly arranged with tendon cells (blue) evenly interspersed and relatively few blood vessels (arrows). B) After an injury the collagen fibres rupture, the tissue becomes much more vascular, promoting the arrival of inflammatory blood cells. The tendon cells themselves also multiply to start the process of rebuilding the damaged structure.
After a tendon injury occurs, horses need time off work with a period of box rest. Controlled exercise is then introduced, which is built up slowly to allow a very gradual return to work. This controlled exercise is an important element of the rehabilitation process, as evidence suggests that exposing the tendon to small amounts of strain has positive effects on the remodelling phase of tendon healing. However, depending on the severity of the initial injury, it can take up to a year before a horse can return to racing. Furthermore, when tendon injuries heal, they repair by forming scar tissue instead of regenerating the normal tendon tissue. Scar tissue does not have the same strength and elasticity as the original tendon tissue, and this makes the tendon susceptible to re-injury when the horse returns to work. The rate of re-injury depends on the extent of the initial injury and the competition level that the horse returns to, but re-injury rates of up to 67% have been reported in racing thoroughbreds. The long periods of rest and the high chance of re-injury therefore combine to make tendon injuries the most common veterinary reason for retirement in racehorses. New treatments for tendon injuries aim to reduce scar tissue formation and increase healthy tissue regeneration, thereby lowering the risk of horses having a re-injury and improving their chance of successfully returning to racing.
Over the past 15 years, the use of stem cells to improve tendon regeneration has been investigated. Stem cells are cells which have the remarkable ability to replicate themselves and turn into other cell types. Stem cells exist from the early stages of development all the way through to adulthood. In some tissues (e.g., skin), where cells are lost during regular turnover, stem cells have crucial roles in normal tissue maintenance. However, in most adult tissues, including the tendon, adult stem cells and the tendon cells themselves are not able to fully regenerate the tissue in response to an injury. In contrast, experimental studies have shown that injuries to fetal tissues including the tendon, are capable of undergoing total regeneration in the absence of any scarring. At the Animal Health Trust in Newmarket, we have an ongoing research project to identify the differences between adult and fetal tendon cells and this is beginning to shed light on why adult cells lead to tendon repair through scarring, but fetal cells can produce tendon regeneration. Understanding the processes involved in fetal tendon regeneration and adult tendon repair might enable new cell based and/or therapeutic treatments to be developed to improve tendon regeneration in adult horses.
In many tissues, including fat and bone marrow, there is a population of stem cells known as mesenchymal stem cells (MSCs). These cells can turn into cells such as bone, cartilage and tendon in the laboratory, suggesting that they might improve tendon tissue regeneration after an injury. MSC-based therapies are now widely available for the treatment of horse tendon injuries. However, research has demonstrated that after injection into the injured tendon, MSCs do not turn into tendon cells. Instead, MSCs produce factors to reduce inflammation and encourage better repair by the tissue’s own cells. So rather than being the builders of new tendon tissue, MSCs act as the foreman to direct tissue repair by other cell types. Although there is some positive data to support the clinical application of MSCs to treat tendon injuries in horses, placebo controlled clinical trial data is lacking. Currently, every horse is treated with its own MSCs. This involves taking a tissue biopsy (most often bone marrow or adipose tissue), growing the cells for 2-4 weeks in the laboratory and then injecting them into the site of injury. This means the horse must undergo an extra clinical procedure. There is inherent variation in the product, and the cells cannot be injected immediately after an injury when they may be the most beneficial.
To allow the prompt treatment of a tendon injury and to improve the ability to standardise the product, allogeneic cells must be used. This means isolating the cells from donor horses and using them to treat unrelated horses. Experimental and clinical studies in horses, mice and humans suggest that this is safe to do with MSCs, and recently an allogeneic MSC product was approved for use in the EU for the treatment of joint inflammation in horses. These cells are isolated from the circulating blood of disease-screened donor horses and are partially turned into cartilage cells in the laboratory. They are then available “off the shelf” to treat unrelated animals. Allogeneic MSC products for tendon injuries are not yet available, but this would provide a significant step forward as it would allow horses to be treated immediately following an injury. However, MSCs exhibit poor survival and retention in the injured tendon and improvements to their persistence in the injury site, and with a better understanding of how they aid tissue regeneration, they are required to enable better optimised therapies in the future.
Our research has previously derived stem cells from very early horse embryos (termed embryonic stem cells, ESCs. Figure 2). ESCs can grow in the laboratory indefinitely and turn into any cell type of the body. These properties make them exciting candidates to provide unlimited numbers of cells to treat a wide range of tissue injuries and diseases. Our experimental work in horses has shown that, in contrast to MSCs, ESCs demonstrate high survival rates in the injured tendon and successfully turn into tendon cells. This suggests that ESCs can directly contribute to tissue regeneration.
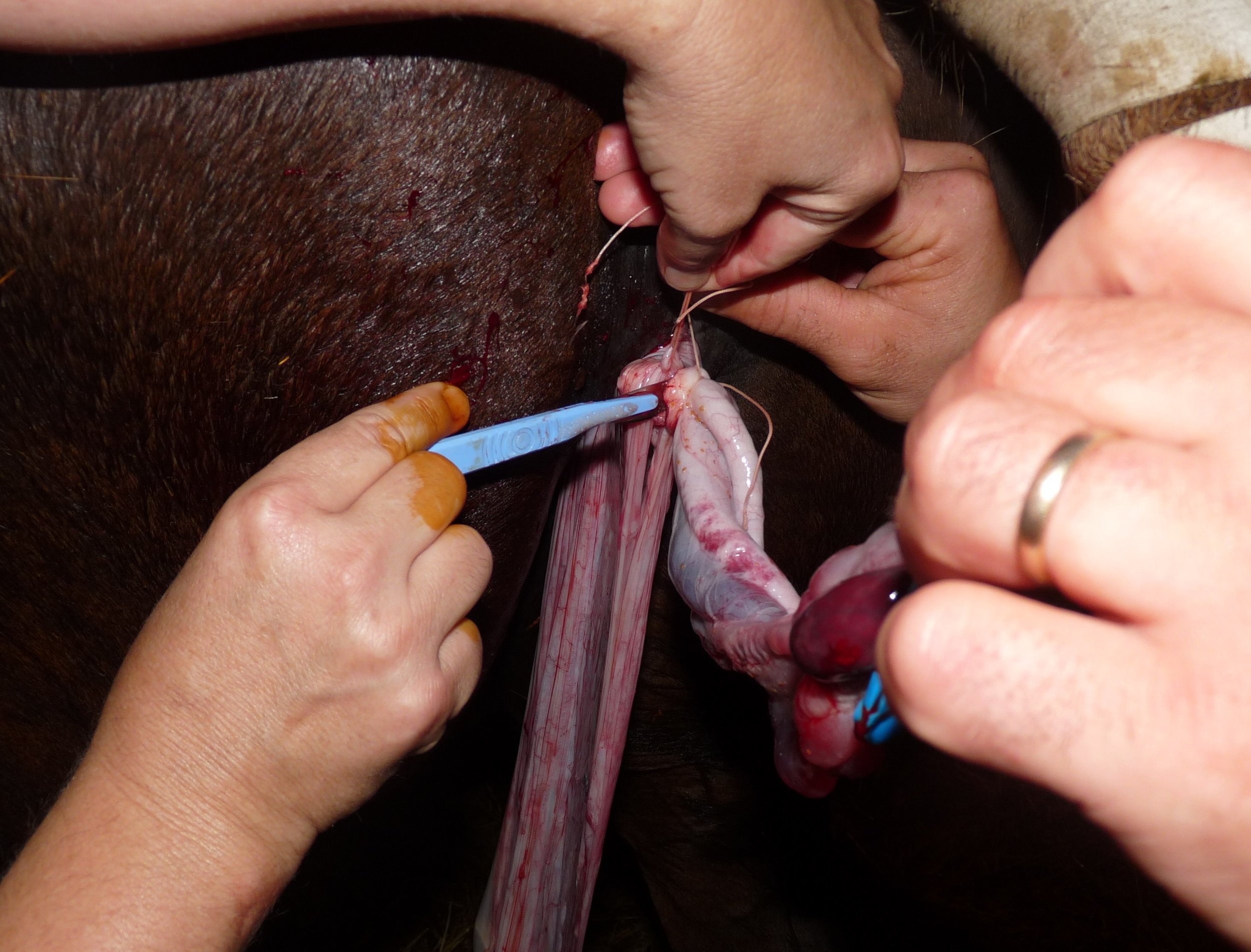
Figure 2. A) A day 7 horse embryo used for the isolation of ESCs. Embryos at this stage of development have reached the mare’s uterus and can be flushed out non-invasively. B) “Colonies” of ESCs can grow forever in the laboratory.
To understand if ESCs can be used to aid tendon regeneration, they must be shown to be both safe and effective. In a clinical setting, ESC-derived tendon cells would be implanted into horses that were unrelated to the original horse embryo from which the ESCs were derived. The recipient horse may therefore recognise the cells as “foreign” and raise an immune response against them. Using laboratory models, we have shown that ESCs which have been turned into tendon cells do not appear recognisable by the immune cells of unrelated horses. This may be due to the very early developmental stage that ESCs originate from, and it suggests that they would be safe to transplant into unrelated horses.
To determine if ESCs would be effective and improve tendon regeneration, without the use of experimental animals, we have established a laboratory system to make “artificial” 3D tendons (Figure 3).
Figure 3. Artificial 3D tendons grown in the laboratory are used to study different sources of tendon cells and help us work out how safe and effective an ESC-based therapy will be. A) Artificial 3D tendons are 1.5 cm in length. B) a highly magnified view of a section through an artificial tendon showing well-organised collagen fibres in green and tendon cells in blue.
ESC-tendon cells can produce artificial 3D tendons just as efficiently as adult and fetal cells, and this system allows us to make detailed comparisons between the different cell types.
BUY THIS ISSUE IN PRINT OR DOWNLOAD —
WHY NOT SUBSCRIBE?